When you have psoriasis, your body produces skin cells too quickly. The skin cells begin to pile up on the surface of the skin, causing plaques and patches to develop.
Psoriasis doesn’t have a cure, but you can learn how to manage the symptoms and avoid triggers. Start with a visit to the dermatologist to find out what kind of psoriasis you have and how to manage it.
What psoriasis looks like
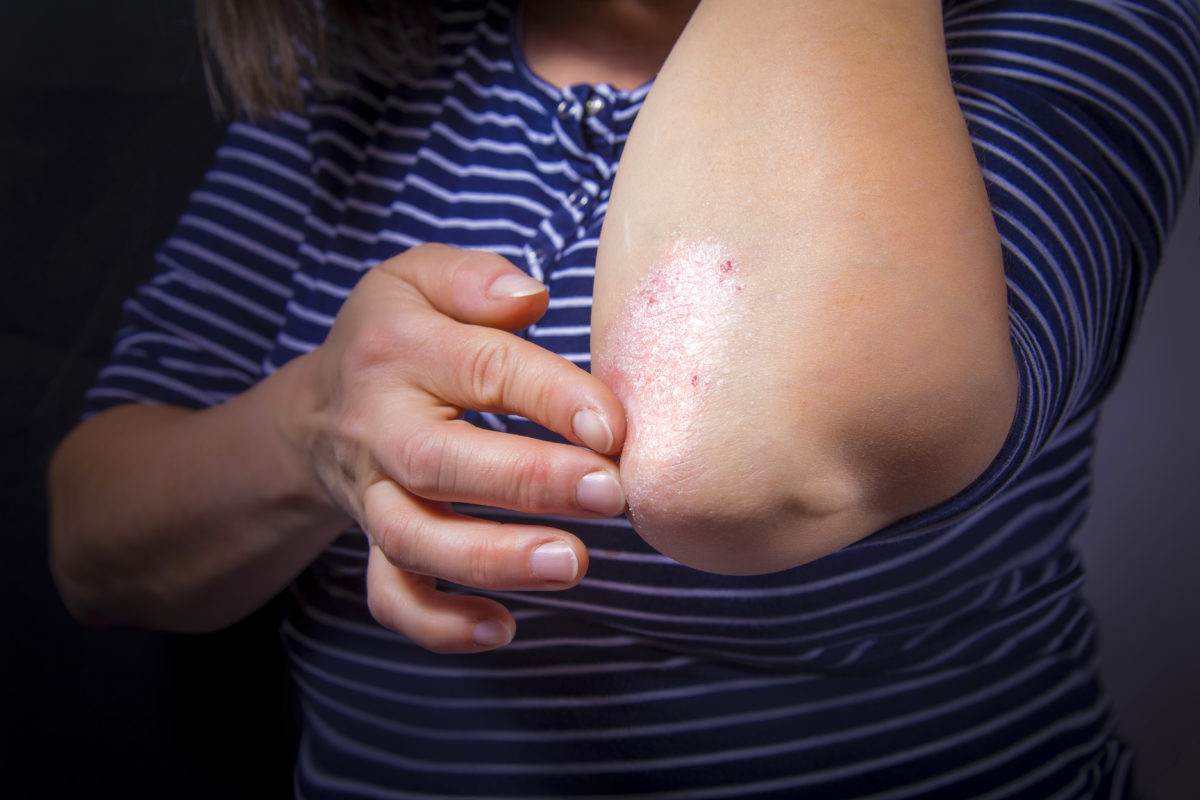
There are several types of psoriasis but the most common is plaque psoriasis. Experts estimate that 80-90% of people with psoriasis have this type. Plaque psoriasis is characterized by thick scaly patches on top of the skin, some with a white coating over them. Sometimes, the skin itches and can get dry and cracked, and might even bleed.
Other kinds of psoriasis include:
- Guttate. Tiny, scaly, pink bumps develop all over the skin, often on the torso or arms and legs. They can last a few weeks or a few months.
- Inverse. Red patches, which can be sore, develop in areas with creases in your skin, like your armpits or groin.
- Pustular. Pus-filled bumps develop on the feet or hands. The skin may be red and swollen, and it’s often very painful.
- Erythrodermic. A painful, peeling red rash develops, which can itch or burn. It’s unusual but when it develops, this inflammatory psoriasis can spread rapidly across the whole body rapidly. It can also cause life-threatening complications.
- Nail psoriasis. About half of people with plaque psoriasis notice the psoriasis also affects their nails, often as tiny pits or discoloration. Sometimes the skin cells will pile up under the nails, raising them up.
The kind of treatment your doctor recommends will depend on your diagnosis — and how severe your psoriasis is. You might find relief from an ointment or steroid cream, or light therapy might be appropriate. Some people need a stronger medication, like cyclosporine or methotrexate, but those are often reserved for severe cases, due to potential side effects.
Risk factors for developing psoriasis
Anyone can develop psoriasis. It can develop at any age, although it most commonly shows up between the ages of 15 and 25. But certain factors increase your chances of developing one (or more kinds):
- Family history. If either of your parents have psoriasis, you’re much more likely to develop it, too.
- Obesity. Research shows that obesity increases your chances for developing psoriasis, although experts aren’t sure why.
- Certain infections. Certain chronic infections, like HIV, or recurring infections like strep throat can make you more vulnerable.
Common triggers for flare-ups
Most people with psoriasis notice that some things just make their psoriasis worse. Your doctor will probably talk to you about your triggers and why you should avoid them. Consider these common triggers:
- Stress. Stress is one of the biggest triggers for psoriasis flare-ups. It’s easier said than done, but if you can find ways to reduce your stress levels, your skin will thank you.
- Injury to your skin. A cut, bite, or scrape can cause trauma to your skin and also trigger a flare. Even a sunburn can do it.
- Certain medications. If you’re taking prednisone, lithium, or certain other meds, watch out for possible flares.
- Smoking. Tobacco use is associated with both the development of psoriasis and flare-ups of the disease. So are many other health conditions, like cardiovascular disease and lung cancer.
- You may want to be careful about your alcohol use if a beer or glass of wine is one of your psoriasis triggers.
- Some people dread the winter, because cold air or cold, dry air makes their psoriasis worse. Others are sensitive to the sun. You may need to cover up or use moisturizers to soothe your skin. Click here to learn more about caring for your skin in cold weather.
One of the most effective ways to manage your psoriasis is to prevent flare-ups before they can occur. So take deliberate steps to avoid anything you notice making your psoriasis worse.
The link to psoriatic arthritis
Psoriasis can go beyond your skin, too. It can affect your joints, making them swollen and painful. About 10-30% of people with psoriasis develop this condition, known as psoriatic arthritis. (Already having psoriasis and a family history of the condition are the biggest risk factors.) And for many of them, it’s a painful problem that affects their daily lives.
Psoriatic arthritis can affect any joint in the body, and it can affect many joints at once. Sore, swollen joints are common, but it can also affect your feet, heels, and your lower back. People with mild psoriatic arthritis may find enough relief from an NSAID (non-steroidal anti-inflammatory drug like ibuprofen or naproxen), but people with more severe symptoms may need stronger medications.
It’s important to not ignore the symptoms and talk to your doctor about the best possible treatment. Left untreated, psoriatic arthritis can cause permanent damage to those affected joints.
Other possible complications related to psoriasis
Psoriasis also raises your risk of developing other health conditions. It’s also associated with a higher prevalence of conditions like cardiovascular disease, high blood pressure, type 2 diabetes, and eye conditions like conjunctivitis and uveitis. Some people with psoriatic arthritis can also develop a rare condition called arthritis mutilans. The disease wears away at the small bones in your hand, eventually deforming them.
While there’s no cure for psoriasis or psoriatic arthritis, your doctor can help you manage them. If your current plan isn’t working, ask your doctor to find a different treatment that works better for you.
Get more information about specific health terms, topics and conditions to better manage your health on bcbst.com. BlueCross BlueShield of Tennessee members can access wellness-related discounts on fitness products, gym memberships, healthy eating and more through Blue365®. BCBST members can also find tools and resources to help improve health and well-being by logging into BlueAccess and going to the Managing Your Health tab.


WellTuned provides inspiration and practical advice for healthy living.
WellTuned does not offer medical advice. Any personal health questions should be addressed to your doctor.